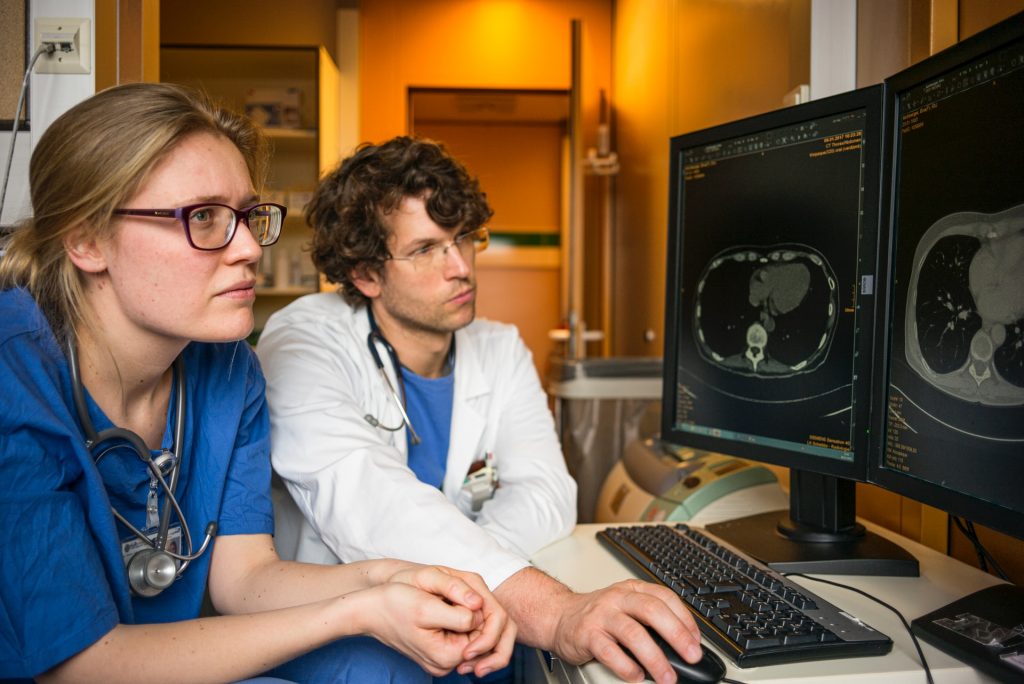
A steady and concerning pattern has emerged in the medical community: an undeniable shortage of doctors. Some estimates say that by 2033, our nation’s physician shortage will be somewhere between 54,000 and 139,000. What are the potential causes, what does it mean for our country’s people, and what can we do to rectify it?
Let’s explore.
The Doctor Shortage: What Went Wrong?

First, we must consider generational factors. Some research says that more than half of all registered nurses are 50 years of age or older. More than half of active physicians are 55 years of age or older, on their way to retirement.
We have an aging medical workforce that can’t keep up with our general population — with a life expectancy that is increasing, meaning that people need more care later into their lives.
To make matters worse, baby boomers — only recently taken over by millennials as the largest population — are also aging and increasingly needing medical care for their worsening conditions.
Next, there’s the fact that medical schools notoriously accept very few students. While the percentage of students they accept has increased slightly over the years, acceptance rates are still startling low — an average of 7%.
The cost of medical school is certainly a hindrance, totaling somewhere in the neighborhood of $338,000 for four years at a private medical school. It’s an incredibly expensive, very long road to becoming a doctor.
And, while the cap on acceptance rates might be moving in the right direction, the cap on residency training hasn’t really budged. Aspiring physicians will still experience a noticeable bottleneck once they get to that stage.
Many people don’t realize that the number of doctors is largely determined by Congress. Every year, the CMS (Centers for Medicare & Medicaid Services) provides funding to hospitals for hiring residents. In other words, Congress has a huge say in the number of new physicians entering the field each year.
This funding amount has hardly moved in a couple of decades.
It doesn’t help that physicians commonly experience burnout (more than half of physicians, by modest estimates), depression (three times more than the general population), and higher rates of suicide than the general population (roughly twice).
These conditions don’t only affect the doctors themselves. Doctors suffering from burnout might be twice as likely to make medical errors, compared to doctors who are healthy, rested, and happy.
Why would students knowingly spend roughly a decade and hundreds of thousands of dollars getting into a field that wears down its professionals?
These certainly aren’t the only causes of the doctor shortage, but they’re some of the more prominent ones. Now, what kinds of ramifications are we dealing with?
What the Physician Shortage Means for Our Nation
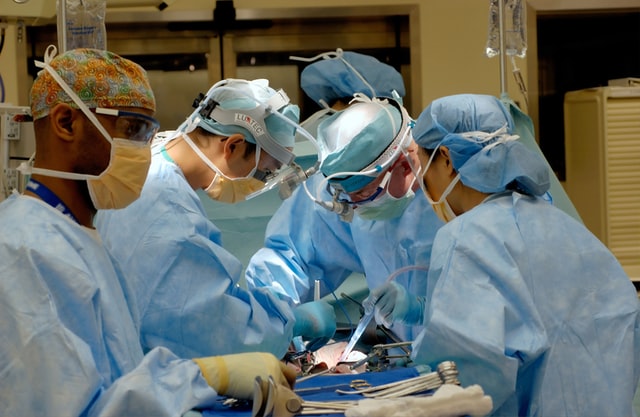
If anything has highlighted our nation’s shortage of physicians, it’s the COVID-19 pandemic. But even outside of the pandemic, it was and will continue to be a huge problem.
An older generation of doctors aging out of their profession ultimately means an age disparity in the remaining physicians — which also means a disparity in experience.
We have more students than ever pursuing a career in medicine as nurses and physician assistants, as opposed to becoming doctors. Specifically, more millennials are opting to become PAs and not doctors, helping to make it one of the fastest growing professions.
To be clear, these are perfectly respectable careers, and they’re roles we need filled.
However, we still need to confront the question: If more people want to become doctors, how can we make it possible for them to become doctors? More on this later.
An insufficient number of doctors means a lower quality of care, further time constraints on the interactions between doctors and patients (which is already a growing problem), an increasingly stressful workload for other healthcare practitioners, longer waits in between visits, and most likely, increased costs for patients.
With medical school and residency taking a minimum of seven years, we’re already behind schedule. The time to act was years ago — but, better late than never. What can we do to improve the physician shortage?
What Can We Do to Improve the Doctor Shortage?

There are a number of actions that we can take to improve the situation.
First, we need to reconsider medical school and residency program acceptance rates, which means reconsidering how much we give programs in funding.
While maintaining the highest standards and imposing rigorous education and training on aspiring doctors, we need to simultaneously find a way to make medical school more affordable and attainable for the people who want it.
We should also rethink how licensing works, making it easier for doctors to move from state to state — something that Arizona has already started and seen success with.
Additionally, we need to significantly improve the conditions under which physicians work. Of course, this partly stems from simply having enough doctors so that individuals aren’t needing to work unsafe and unhealthy hours. However, considering the incredibly sensitive nature of the services that doctors provide, we need to be especially cognizant of helping them establish a better work-life balance. It’s vital not only to their well-being, but also to the quality of service they’re able to provide to their patients.
It’s a long road ahead, and no action that we take can fix things overnight. It’s going to take months and years of change from students, professionals, and policymakers to alter the direction in which things are headed.
But if we can do that, we’ll see a more fulfilled population of physicians who are better able to serve their communities, and a steadier influx of students and residents.













